| . |  |
. |
| . |  |
. |
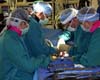
Fort Detrick MD (AFNS) May 16, 2006 However science fiction-esque it may have sounded decades ago, using robots to perform delicate surgeries is decidedly science fact today. Looking toward future decades, researchers are now trying to find ways to take robotic surgery to the battlefield. "We're not talking about something that's going to be immediately available, but if we don't do this research now, we will not have the option of having surgical intervention remotely or robotically (on the battlefield). That's the underpinning motivation for our getting into it," said Dr. Gerry Moses of the Telemedicine and Advanced Technology Research Center. The basics A surgeon using a robotic surgery system in a hospital typically sits across the room from a patient. Looking through a three-dimensional monitor, the surgeon uses a joystick to control the robot, which is armed with surgical tools and a camera. A subset of laparoscopic surgery, robotic surgeries are great for minimally invasive procedures, said Col. Noah Schenkman, chief of urology service at the Walter Reed Army Medical Center. In the past three years, he has performed almost 50 operations using a robotic surgery system to repair blockages between the kidney and the ureter, or to remove the prostate. "Lap instruments are very current, but sometimes they're not very ergonomic. They don't allow you to make the complex, difficult maneuvers that you can make with just your hands," he said. "The robot allows you to regain some of those complex movements because it has an articulating instrument that allows you to make those movements, (like) sewing, during reconstructive operations." Schenkman said robotic surgery offers a surgeon several benefits. Because it's a machine, it eliminates the normal tremor associated with human hands performing fine motor movements. The system's 3-D view also gives the operator increased vision and magnification, both of which are important in complex, intricate surgeries. And because the surgery is done from a sitting position, it's doesn't wear out the surgeon. "It's a little easier to do live maneuvers if you're in a comfortable sitting position," he said. "Sometimes you're in an awkward standing position with some of the other laparoscopic cases." Because of the benefits robotic surgery offers, researchers at the Telemedicine and Advanced Technology Research Center want to bring it to the battlefield and have imagined how it would play out. "We're talking years out now," Moses said. "We're not talking about something that's going to be immediately available." In a futuristic Defense Advanced Research Projects Agency, or DARPA, video, a scenario unfolds where a Soldier radios that a man's down. Within seconds an unmanned evacuation vehicle pulls the wounded Soldier onto a stretcher and transports him to a surgical suite inside the vehicle. The Soldier's body is scanned for injury and a diagnosis is made. Surgery commences and is completed, then an unmanned aerial vehicle appears and evacuates the Soldier. According to the DARPA Web site, that system, called the Trauma Pod, will move forward incrementally. One of its first steps is replacing scrub nurses in the operating room. At a conference in January, Moses told attendees just how close that vision is to becoming a reality. Meet Penelope To further the concept of an operating room void of all people except for the patient, the Telemedicine and Advanced Technology Research Center funded an idea that surgeon Dr. Michael Treat of Columbia University had for a robotic scrub nurse. Named "Penelope," the robot is charged with handing requested instruments to the surgeon as well as keeping count of them. "When I first saw Penelope, it was slow. It handled five instruments, and there was a delay period between the time he (Treat) said what he wanted and what he got," Moses said. After three years of refinements, Penelope is much improved. It now responds verbally and can accurately image and retrieve 14 instruments when requested. Penelope first assisted with a human surgery in 2005. "This is a terrific example of technology development," he said. "If you don't invest in the slow, draggy four- or five-instrument-effort at one point, three years later you're not going to have a robotic scrub assistant." Remote surgeries Robotic telesurgeries from long distances are making steady progress, Moses said, but are in a "very experimental time period." In 2001, though he was physically in New York, Dr. Jacques Marescaux removed a gallbladder from a 68-year-old woman in Strasbourg, France, marking the first-ever transatlantic telesurgery. "It did demonstrate the possibility of remote intervention surgery," Moses said, adding that many safeguards were put in place for that procedure, including a back-up surgical team waiting to intervene and a dedicated transatlantic line to ensure continuous signal connection. As another success story, Moses offers the example of Canadian telesurgeon, Dr. Mehran Anvari, who has performed more than two dozen telesurgeries from Ontario on patients who are nearly 250 miles away. Anvari, a scientific partner with the Telemedicine and Advanced Technology Research Center, uses a specially configured laparoscopic robot that measures and transmits the movements of his hands and fingers to perform minimally invasive surgeries on stomachs, kidneys and spleens. "None are as complicated as brain or heart surgeries, but every time he conducts a successful surgery, he is reinforcing the point that telesurgery is possible," Moses said. Challenges Though the accuracy and efficiency of robotic controls have improved tremendously, several technology hurdles still need to be cleared before robotic telesurgeries become a mainstay in medicine, Moses said. The issues of latency - the delay in the transmission of what happens at one end and what happens at the other end - and jitter - the interrupted transmission of the electronic signal - can make the difference between a successful and disastrous operation. "This is where we at TATRC have been focusing our investment in research," Moses said. "We are trying to identify how to overcome those technical challenges associated with an enhanced robotic surgical system." To show how their work is progressing, the Telemedicine and Advanced Technology Research Center conducted a live robotic telesurgery over the Internet at a conference in April 2005. In Denver, a surgeon with the master controls operated on two pig patients in Sunnyvale, Calif., where the slave controls were overseen by a senior resident. To overcome the latency and jitter, engineers refined the electrical signal for the last 40 feet at each end. "Whatever latency remained was in a tolerable limit for the surgeon to accomodate that minimal delay between seeing a television image showing him what was happening in Sunnyvale versus what his hands were doing in Denver," Moses said. "That demonstration made the case for us that telesurgery was a resource for us in healthcare as we go forward." In addition to latency and jitter, a robotic telesurgery system would face other practical limitations as well, said Col. John Holcomb, a trauma surgeon who has deployed seven times to Operation Iraqi Freedom. "The lights still go out in the ORs in Iraq, and communication is exquisitely difficult," he said. Moses and his partners are also taking on the robots' design. Commercial systems, like the one Schenkman uses at WRAMC, in many ways violate the military's mantra of smaller, lighter and less power for items that go in the field. The system at WRAMC, is "heavy, large, bulky and takes a lot of space up and is very resource intensive," Schenkman said. "It takes a lot of expertise to keep it up and maintain it. If it broke it would be hard to get the repairman to come and fix it out there (on the battlefield)." The initiative to make surgical robots smaller has already begun, in part because NASA is exploring telesurgery for its use in remote locations, like space. In 2005, an astronaut in NASA's Aquarius Underwater Laboratory in the Gulf of Mexico was telementored - essentially coached via video and audio links - by Anvari in the art of suturing and other surgical tasks. This year, the Aquarius project will take another step forward as Anvari in Canada performs a robotic surgery inside the Aquarius supported by another surgeon inside the Aquarius laboratory. For that to occur, however, the robot had to be scaled down quite a bit. "We had to develop a smaller, more portable and efficient robotic slave system, referred to as the Army Arm, that could be used in this remote setting and could be linked electronically via the Internet with Dr. Anvari's master console in Canada," Moses said. Telementoring, telecollaborations At the American Telemedicine Association conference this month, Moses said a "true telecollaboration" will take place where multiple surgeons will operate the instruments. "We're going to connect additional sites to the robotic system so the patient may be in one location, a surgery team in one location and another surgery team in a third location that won't just telementor, but can actually interact with the instruments collaboratively and operate on the pig together," Moses said. "We've had demonstrations where we watched surgeons before. What is different about the plan that we have for this spring is the true collaborative nature, rather than just telementoring or telewatching." For battlefield surgery in the future, Schenkman can foresee telecollaboration, where a remote surgeon can assist a deployed surgeon who doesn't have expertise in a particular procedure. "It's not going to be the DARPA video with the robot that does the surgery by itself," he said. "To actually have a surgeon from far away do this is not going to work because someone has to put the instruments into the patient. You're going to have to have some sort of surgical expertise in theater, where the patient is." Whether patients will accept robotic telesurgery remains to be seen. Schenkman said he wouldn't volunteer to be the first patient. Moses, who has had two cataract surgeries, said he would trust his ophthalmologist to perform that telesurgery robotically. "It's a matter of confidence in the surgeon," he said. "If you're a casualty on a battlefield, you don't ask the question. Whoever you've got is fine." (Editor's note: Karen Fleming-Michael writes for the U.S. Army Medical Research and Materiel Command.) Related Links the missing link
 Offutt NE (AFPN) May 16, 2006
Offutt NE (AFPN) May 16, 2006Reshaping medical career fields as lean, efficient tools for providing 21st century healthcare is a priority for the Air Force deputy surgeon general. |
|
| The content herein, unless otherwise known to be public domain, are Copyright 1995-2006 - SpaceDaily.AFP and UPI Wire Stories are copyright Agence France-Presse and United Press International. ESA PortalReports are copyright European Space Agency. All NASA sourced material is public domain. Additionalcopyrights may apply in whole or part to other bona fide parties. Advertising does not imply endorsement,agreement or approval of any opinions, statements or information provided by SpaceDaily on any Web page published or hosted by SpaceDaily. Privacy Statement |